Newly discovered esophagus stem cells grow into transplantable tissue
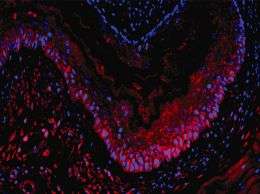
Researchers at the University of Pennsylvania School of Medicine have discovered stem cells in the esophagus of mice that were able to grow into tissue-like structures and when placed into immune-deficient mice were able to form parts of an esophagus lining. The investigators report their findings online this month in the Journal of Clinical Investigation.
"The immediate implication is that we'll have a better understanding of the role of these stem cells in normal biology, as well as in regenerative and cancer biology," says senior author Anil K. Rustgi, MD, the T. Grier Miller Professor of Medicine and Genetics and Chief of Gastroenterology. "Down the road, we will develop a panel of markers that will define these stem cells and use them in replacement therapy for diseases like gastroesophogeal reflux disease [GERD] and also to understand Barrett's esophagus, a precursor to esophageal adenocarcinoma and how to reverse that before it becomes cancer."
Diseases of the esophagus are very common in the United States and worldwide. "Benign forms include GERD and millions are affected," notes Rustgi.
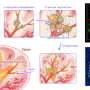
GERD can sometimes lead to inflammation of the esophagus, called esophagitis. "In some of these cases esophagitis can lead to a swapping of the normal lining of the esophagus with a lining that looks more like the intestinal lining and that's called Barrett's esophagus," explains Rustgi. "This can lead to cancer of the esophagus, which is the fastest rising cancer in the US, increasing by 7 to 8 percent a year."
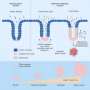
The researchers set out to identify and characterize potential stem cells--those with the ability to self renew--in the esophagus to understand normal biology and how injured cells may one day be repaired.
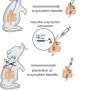
First, they grew mouse esophageal cells they suspected were adult stem cells. Those cells formed colonies that self renewed. These cells then grew into esophageal lining tissue in a three-dimensional culture apparatus. "These tissue culture cells formed a mature epithelium sitting on top of the matrix," says Rustgi. "The whole construct is a form of tissue engineering."
The investigators then tested their pieces of esophageal lining in whole animals. When the tissue-engineered patches were transplanted under the skin of immunodeficient mice, the cells formed epithelial structures. Additionally, in a mouse model of injury of the esophagus in a normal mouse, which mimics what happens during acid reflux, green-stained stem cells migrated to the injured lining cells and co-labeled with the repaired cells, indicating involvement of the stem cells in tissue repair and regeneration.
Eventually the researchers will develop genetically engineered mouse models to be able to track molecular markers of esophageal stem cells found in a micorarray study. The group has already developed a library of human esophageal cell lines and is looking for human versions of markers already identified in mice.
Source: University of Pennsylvania