Short RNA strand helps exposed skin cells protect body from bacteria, dehydration and even cancer
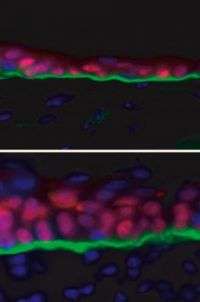
Every minute, 30,000 of our outermost skin cells die so that we can live. When they do, new cells migrate from the inner layer of the skin to the surface of it, where they form a tough protective barrier. In a series of elegant experiments in mice, researchers at Rockefeller University have now discovered a tiny RNA molecule that helps create this barrier. The results not only yield new insight into how skin first evolved, but also suggest how healthy cells can turn cancerous.
Hundreds of these tiny RNA molecules, called microRNAs, are expressed in skin, "But there was something curious about one in particular, microRNA-203," says Rui Yi, a postdoc who works with Elaine Fuchs, head of the Laboratory of Mammalian Cell Biology and Development. "As an embryo develops, the expression of microRNA-203 jumps very quickly over just two days. From being barely detectable at day 13, this microRNA becomes the most abundant expressed in skin," says Yi, whose work will be published as an advance online publication in Nature March 2. MicroRNAs, which were discovered in mammals in 2001, regulate genes outside of the cell's nucleus.
Yi and Fuchs, who is also a Howard Hughes Medical Institute investigator and Rebecca C. Lancefield Professor at Rockefeller, found that during the 13th day of development, mouse skin is primarily composed of undifferentiated stem cells. Two days later, these stem cells exit the inner layer of the skin and begin to differentiate into cells that form the outermost, protective layer. MicroRNA-203's expression skyrockets precisely during this period, suggesting that it plays some key role in the barrier's development.
In order to figure out its role, Yi and Fuchs needed to pinpoint exactly where microRNA-203 is expressed. Other microRNAs have been found to be specific to heart and muscle tissues; some exist almost exclusively in the brain. However, this microRNA was found only in very specific types of skin -- stratified epithelial tissues, to be exact -- and only in this skin type's outer layers. What's more, this expression pattern is identical to that found in humans, zebrafish, chickens and the like -- in other words, vertebrates that evolved more than 400 million years apart.
"If it has been expressed in this very specific tissue for a long time and across several species, it means that it probably plays an important role there," says Yi. To find out its function, Yi, in one set of experiments, used a genetic technique to precociously express microRNA in the inner layer of the skin, where stem cells proliferate at a fast clip. In a second set of experiments, he blocked microRNA-203 from functioning in the outer layer using an antagomir, a molecule that binds directly to microRNA-203 and shuts down its ability to carry out its function.
In the first set, he found that the stem cells proliferated significantly less than they did when microRNA-203 wasn't expressed, and, as a result, the mice formed very thin skin -- hardly a protective layer at all. The stem cells, the researchers saw, lost their ability to proliferate not because microRNA-203 killed them off but because it suppressed the activity of a molecule called p63, whose job is to keep cells, primarily stem cells, proliferating. In the second set of experiments, Yi found that the cells in the outer layer proliferated significantly more than they did when microRNA-203 was expressed. The reason: because microRNA-203 wasn't available to shut down p63's busy work.
"We found that microRNA-203 acts to stop the translation of the p63 protein," says Fuchs. "The result is a swift transition from proliferating stem cells within the innermost layer of the epidermis and terminally differentiating cells as they exit this layer and move outward to the skin surface."
The findings have intriguing implications for cancer, since p63 is found in excess in cancer cells. "As a next step, we are going to examine whether low expression of microRNA-203 is associated with squamous cell carcinomas," says Fuchs, "and whether by putting back microRNA-203 we can inhibit the growth of these cancer cells."
Source: Rockefeller University