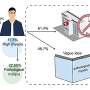
Relationship between environmental stress and cancer elucidated
One way environmental stress causes cancer is by reducing the activity level of an enzyme that causes cell death, researchers say.
They found that stress-inducing agents, such as oxidative stress, recruit a protein called SENP1 that cuts a regulator called SUMO1 away from the enzyme SIRT1 so its activity level drops, says Dr. Yonghua Yang, postdoctoral fellow in the laboratory of Dr. Kapil Bhalla, director of the MCG Cancer Center.
This fundamental finding about the relationship between stress and cancer opens the door for treatments that increase SENP1 activity, making it easier for cells that are becoming cancerous to die, says Dr. Yang, first author on a paper published in the November issue of Nature Cell Biology.
“This is one of the things that makes cancer cells so durable, one way they survive so well,” says Dr. Yang. “We want to see if we can block that process and make cells die.” Increased SIRT1 activity – which is routinely present in cancer – even makes cancer cells more resistant to anticancer drugs such as chemotherapy.
The complication is that decreasing programmed cell death, or apoptosis, increases longevity, says Dr. Yang. However he now has evidence that SIRT1 – also under study for its longevity role – has different targets when it comes to cancer promotion and longevity that will provide distinct targets for manipulating each.
“Whether apoptosis is good or bad depends on the circumstances,” says Dr. Yang. “But it’s good for cancer therapy.”
“This paper describes how stress causes desumoylation and sumoylation of SIRT1 and ultimately cancer,” says Dr. Bhalla, Cecil F. Whitaker Jr., M.D./Georgia Research Alliance Eminent Scholar in Cancer and a study co-author.
“Stress-inducing agents produce the association of this enzyme,SIRT-1, with the desumoylating enzyme, SENP1, so cells become more resistant to stress-induced apoptosis,” says Dr. Bhalla. “Once SIRT1 is desumoylated, it’s less active and you want its activity.” When SIRT1 is less active, p53, a tumor suppressor gene that also causes apoptosis, becomes more active.
SIRT1, found throughout the body, is a regulator of protein function through a process called acetylation. MCG researchers also found that sumoylation of SIRT1 (combining it with SUMO1) made it more active and sumoylation motif, which enables SUMO1 to combine with SIRT1, is needed to make that happen.
They have added SUMO1 to human cancer cells and increased SIRT1 activity then used SENP1 to cleave it and reduce activity.
Researchers studying the longevity benefits of SIRT1 have found conflicting information in yeast and mice about whether or not SIRT1 is of benefit. Dr. Yang may have found one reason: mice SIRT1 doesn’t contain sumoylation motif. When he created sumoylation motif in mice, SIRT1 activity went up. Dr. Yang will do follow up studies to see if these mice live longer but says SIRT1 may simply have a different function in mice than in humans or yeast, also a common research model.
Source: Medical College of Georgia