Potential early warning system for lung cancer identified
An immune system protein could act as an early warning system for lung cancer, reveals research published ahead of print in the journal Thorax.
Lung cancer kills around 900,000 people every year, and can take 20 years or more to develop fully. But it is usually only picked up at an advanced stage, when the chances of successful treatment are slim.
As yet, there is no effective early warning system to detect the disease in its early treatable stages, and the dismal long term prospects of patients with lung cancer have changed little in the past 30 years.
The research team analysed blood (plasma) samples from 50 healthy volunteers and 104 people with different types of lung cancer.
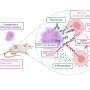
They tested for autoantibodies - immune system proteins directed at the body’s own tissues in response to specific chemical signals in the body.
They looked in particular for a panel of seven autoantibodies, which are associated with ‘solid tumours,’ such a lung, breast, ovarian, and prostate cancers, and triggered when cancerous changes are taking place.
They found the presence of all seven autoantibodies, and very high levels of at least one of the seven in almost eight out of 10 samples taken from patients with confirmed lung cancer.
And these autoantibodies were found in eight out of the nine patients whose cancer had not infiltrated the lymph nodes, the body’s gatekeepers.
This indicates that the disease had not yet spread elsewhere and offers an 80% chance of a cure.
Only one healthy volunteer had more than one of these autoantibodies in their blood.
Other research has indicated that these autoantibodies can be picked up as early as five years before clinical symptoms start to show.
In a previous study, the researchers found abnormally high levels of specific autoantibodies in patients with breast cancer, prompting them to suggest that a test for these could be added to the screening programme. That study also showed that these autoantibodies were present before clinical symptoms appeared..
The authors argue that the lungs are especially sensitive to radiation, so repeated chest x-rays are not ideal for picking up lung cancer.
A blood test, on the other hand, is cheap compared with imaging techniques, and has no side effects. And the panel can be changed to include more or different autoantibodies for lung and other cancers.
They suggest that the blood test could be used for people at increased risk of developing the disease, such as smokers and passive smokers.
If they test positive, these people could then be referred for more detailed scans, such as computed tomography (CT) or magnetic resonance imaging (MRI), they suggest.
Source: British Medical Journal