Researchers Discover Link Between Schizophrenia, Autism and Maternal Flu
A team of California Institute of Technology researchers has found an unexpected link connecting schizophrenia and autism to the importance of covering your mouth whenever you sneeze.
It has been known for some time that schizophrenia is more common among people born in the winter and spring months, as well as in people born following influenza epidemics. Recent studies suggest that if a woman suffers even one respiratory infection during her second trimester, her offspring's risk of schizophrenia rises by three to seven times.
Since schizophrenia and autism have a strong (though elusive) genetic component, there is no absolute certainty that infection will cause the disorders in a given case, but it is believed that as many as 21 percent of known cases of schizophrenia may have been triggered in this way. The conclusion is that susceptibility to these disorders is increased by something that occurs to mother or fetus during a bout with the flu.
Now, researchers have isolated a protein that plays a pivotal role in that dire chain of events. A paper containing their results, "Maternal immune activation alters fetal brain development through interleukin-6," will be published in the Oct. 3 issue of the Journal of Neuroscience.
Surprisingly, the finger of blame does not point at the virus itself. Since influenza infection is generally restricted to the mother's respiratory tract, the team speculated that what acts as the mediator is not the mother's infection per se but something in her immune response to it.
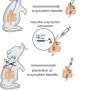
To prove this, they triggered an artificial immune response in pregnant mice--giving them a faux case of the flu. The trigger they used was a snippet of double-stranded RNA called poly(I:C), which fools the immune system into thinking there has been an infection by an RNA virus.
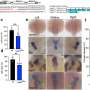
A single, mid-gestation injection of poly(I:C) creates a strong immune response in a pregnant mouse. When her offspring reach adulthood, they display behavioral and tissue abnormalities similar to those seen in schizophrenia in humans.
Though there might be some disagreement over what it means for a mouse to be schizophrenic, these abnormalities are generally marked by inappropriateness of response and difficulty in coping. For instance, afflicted mice often show antisocial tendencies, have trouble internalizing basic cause-and-effect connections, and are anxious about entering wide-open spaces or interacting with novel objects. Moreover, some of these abnormal behaviors are corrected by antipsychotic drug treatment.
These behaviors then pose a new question, what in the mother's immune response caused the abnormalities?
At the cellular level, the innate immune response is driven by proteins called cytokines, which are produced by the body in response to infection. The researchers speculated that something was being transmitted to the fetus by one or more cytokines produced by the mother in response to her infection.
"It's known that humans that are treated--say, for cancer--with an experimental cytokine treatment can display very significant changes in behavior," says Paul H. Patterson, Biaggini Professor of Biological Sciences and senior author of the paper. "So we know cytokines can have dramatic effects, of the kind you see in schizophrenia."
The team tried injecting the pregnant mice with individual cytokines, rather than with poly(I:C). It turned out that after a single dose of a specific cytokine known as interleukin-6 (or IL-6), a mouse would give birth to offspring who, at maturity, exhibited the familiar schizophrenia- and autism-like behaviors.
To confirm the role of IL-6, Steve Smith, the lead researcher, gave fake colds (poly(I:C)) to two groups of pregnant, IL-6-free mice. One group had received anti-IL-6 antibodies which blocked IL-6; the other consisted of so-called IL-6 knockout mice (mice whose genetic makeup prevents them from synthesizing IL-6). In both groups, offspring grew up normal, showing that IL-6 is necessary for the maternal poly(I:C) treatment to alter fetal brain development and subsequent behavior in the offspring.
The decision to try injecting IL-6 was a long shot. "It is really unexpected that a single injection of a single cytokine would exert such a powerful effect," says Patterson.
The scientists are still unsure what it is about increasing IL-6 levels in the mother that causes undesirable effects in her offspring. "The most obvious possibility is that IL-6 acts directly on the fetal brain," the paper's authors say, but they acknowledge that the cytokine might also alter the transfer of materials across the placenta or might even alter the maternal immune system that gave rise to it, in effect triggering a low-grade rejection of the developing fetal tissue by the mother's body.
Once the exact role of IL-6 has been nailed down, there will still be more work to be done. The researchers are hunting for ways of preventing cytokines like IL-6 from inflicting their damage on the developing or maturing brain--perhaps via mechanisms involving other cytokines.
"We could certainly imagine that there would be anti-inflammatory cytokines that would be involved, that would be acting in the opposite direction," suggests Patterson. "We haven't tested those yet, but we would like to. We also want to test anti-inflammatory drugs in the postnatal offspring to see if we can normalize their behavior."
The paper's authors are Patterson and Stephen Smith, a graduate student in biology at Caltech; Jennifer Li, now a graduate student at the University of California Medical Center, San Francisco, who participated in the project as part of a Caltech Summer Undergraduate Research Fellowship; and Drs. Krassimira Garbett and Karoly Mirnics, both of the Department of Psychiatry and the Vanderbilt Kennedy Center for Research on Human Development, Vanderbilt University.
Source: Caltech