Toward understanding the dangers of the fake marijuana called 'Spice' or 'K2'
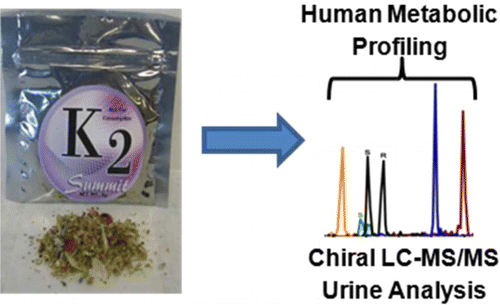
The harmful effects of increasingly popular designer cannabis products called "Spice" or "K2" have puzzled scientists for years, but now a group of researchers is reporting progress toward understanding what makes them so toxic. The study, published in the ACS journal Analytical Chemistry, describes development of a method that could someday help physicians diagnose and treat the thousands of young adults and teens who end up in emergency rooms after taking the drugs.
Jeffery Moran and colleagues note that synthetic marijuana, often marketed as "natural incense," "potpourri," Spice or K2, is a significant public health concern, and 1 in 9 high school seniors admit recent use. The products appear across the United States and Europe, and are the second most popular drug after real marijuana for many American teens and young adults. The substances produce a "high," but also can cause a wide range of dangerous side effects including seizures, hallucinations, severe kidney damage, psychotic behavior and heart attacks. Scientists are quickly playing catch-up to understand how these fake pot products work in order to identify them in users' urine and to treat the devastating health effects, which, in some cases, plague users for months after they initially take it.
To gain insight into the effects of designer marijuana products, Moran's team developed a new method and used it to study how the body processes two popular forms in Spice and K2, known as JWH-018 and AM2201. Urine samples from 15 people who tested positive for use showed significant differences in how the individuals' bodies processed the drugs. This finding could help explain why some people experience more severe effects from the drugs than others.
More information: Targeted Metabolomic Approach for Assessing Human Synthetic Cannabinoid Exposure and Pharmacology, Anal. Chem., 2013, 85 (19), pp 9390–9399. DOI: 10.1021/ac4024704
Abstract
Designer synthetic cannabinoids like JWH-018 and AM2201 have unique clinical toxicity. Cytochrome-P450-mediated metabolism of each leads to the generation of pharmacologically active (?)- and (?-1)-monohydroxyl metabolites that retain high affinity for cannabinoid type-1 receptors, exhibit ?9-THC-like effects in rodents, and are conjugated with glucuronic acid prior to excretion in human urine. Previous studies have not measured the contribution of the specific (?-1)-monohydroxyl enantiomers in human metabolism and toxicity. This study uses a chiral liquid chromatography–tandem mass spectroscopy approach (LC–MS/MS) to quantify each specific enantiomer and other nonchiral, human metabolites of JWH-018 and AM2201 in human urine. The accuracy (average % RE = 18.6) and reproducibility (average CV = 15.8%) of the method resulted in low-level quantification (average LLQ = 0.99 ng/mL) of each metabolite. Comparisons with a previously validated nonchiral method showed strong correlation between the two approaches (average r2 = 0.89). Pilot data from human urine samples demonstrate enantiospecific excretion patterns. The (S)-isomer of the JWH-018-(?-1)-monohydroxyl metabolite was predominantly excreted (>87%) in human urine as the glucuronic acid conjugate, whereas the relative abundance of the corresponding AM2201-(?-1)-metabolite was low (<5%) and did not demonstrate enantiospecificity (approximate 50:50 ratio of each enantiomer). The new chiral method provides a comprehensive, targeted metabolomic approach for studying the human metabolism of JWH-018 and AM2201. Preliminary evaluations of specific enantiomeric contributions support the use of this approach in future studies designed to understand the pharmacokinetic properties of JWH-018 and/or AM2201.
Journal information: Analytical Chemistry
Provided by American Chemical Society