December 19, 2011 report
Researchers use whole-genome sequencing to monitor evolution of drug resistance in bacteria
(PhysOrg.com) -- Two research groups working independently have come up with two different ways to use whole-genome sequencing to follow the path bacteria take in developing resistance to anti-bacterial drugs. Such research could prove useful in figuring out ways to stop the evolutionary process, thereby safeguarding current anti-bacterial agents for future patients. Both groups have published papers describing their work in Nature Genetics. The first group has found a way to actually monitor the evolution of the E. coli bacteria over several generations as it’s exposed to three types of anti-bacterial agents. The second group has figured out a way to follow mutations in bacteria that occur after anti-bacterial agents have been discontinued.
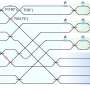
The first group, all working out of Harvard University, created what they call a “morbidostat”; a computer controlled environment that reads signs from a bacteria culture to asses its degree of happiness with its surroundings, then tweaks it just a little bit to make it unhappy. Bacteria that are happy don’t need to adapt, thus, to cause them to evolve, three types of antibacterial agents were introduced into the morbidostat along with the bacteria: chloramphenicol, doxycyclin, and trimethoprim. To see what evolutionary changes were occurring, the team took regular samples and studied them using whole-genome sequencing. Using this technique the team found they could actually watch the bacteria evolve into resistant strains. But of particular note, they found that at least when exposed to trimethoprim, Escherichia coli evolves in very predictable ways, a bit of knowledge that could help doctors stay one step ahead of such changes when treating patients by predicting them before they are able to occur.
Just as interesting is the study undertaken by the second group; a team made up of an international group of researchers. Here the team wanted to know what goes on with bacteria that are subjected to anti-bacterial agents, after the treatment is stopped. Do they stop evolving, or do they keep on doing so as a means of responding to the effects of the drugs?
Prior research has already shown that most often drug-resistant bacteria for some reason don’t grow as quickly as those that aren’t resistant when in an environment free of antibiotics, which should mean resistant strains should have transmission rates that are lower. Unfortunately, this is not always the case as some resistant strains of some types of bacteria have shown an ability to transmit just as quickly as their non-resistant brethren. To find out why this is, the team analyzed both types of strains using whole-genome sequencing to find out exactly what was going with different strains of M. tuberculosis.
The team found that those strains that were both resistant and able to transmit at the same rates as the non-resistant group had developed two types of mutations. The first was, obviously, the changes that had come about that had made them resistant. The second change was the surprise; the bacteria samples had actually evolved in a way that allowed them to regain a high transmission rate, which showed they had continued to evolve after the anti-bacterial drug had been stopped, this time, to get back something it had lost due to the drug.
Taken together, the studies show that by using whole-genome sequencing, researchers are moving ever closer to fully understanding how bacteria mutate and evolve to make themselves resistant to anti-bacterial agents. The hope is that once the entire process is fully understood, new ways to prevent it from happening can be developed.
More information: [1] Whole-genome sequencing of rifampicin-resistant Mycobacterium tuberculosis strains identifies compensatory mutations in RNA polymerase genes, Nature Genetics (2011) doi:10.1038/ng.1038
Abstract
Epidemics of drug-resistant bacteria emerge worldwide, even as resistant strains frequently have reduced fitness compared to their drug-susceptible counterparts. Data from model systems suggest that the fitness cost of antimicrobial resistance can be reduced by compensatory mutations; however, there is limited evidence that compensatory evolution has any significant role in the success of drug-resistant bacteria in human populations. Here we describe a set of compensatory mutations in the RNA polymerase genes of rifampicin-resistant M. tuberculosis, the etiologic agent of human tuberculosis (TB). M. tuberculosis strains harboring these compensatory mutations showed a high competitive fitness in vitro. Moreover, these mutations were associated with high fitness in vivo, as determined by examining their relative clinical frequency across patient populations. Of note, in countries with the world's highest incidence of multidrug-resistant (MDR) TB, more than 30% of MDR clinical isolates had this form of mutation. Our findings support a role for compensatory evolution in the global epidemics of MDR TB.
Evolutionary paths to antibiotic resistance under dynamically sustained drug selection, Nature Genetics (2011) doi:10.1038/ng.1034
Abstract
Antibiotic resistance can evolve through the sequential accumulation of multiple mutations. To study such gradual evolution, we developed a selection device, the 'morbidostat', that continuously monitors bacterial growth and dynamically regulates drug concentrations, such that the evolving population is constantly challenged. We analyzed the evolution of resistance in Escherichia coli under selection with single drugs, including chloramphenicol, doxycycline and trimethoprim. Over a period of ~20 days, resistance levels increased dramatically, with parallel populations showing similar phenotypic trajectories. Whole-genome sequencing of the evolved strains identified mutations both specific to resistance to a particular drug and shared in resistance to multiple drugs. Chloramphenicol and doxycycline resistance evolved smoothly through diverse combinations of mutations in genes involved in translation, transcription and transport. In contrast, trimethoprim resistance evolved in a stepwise manner, through mutations restricted to the gene encoding the enzyme dihydrofolate reductase (DHFR). Sequencing of DHFR over the time course of the experiment showed that parallel populations evolved similar mutations and acquired them in a similar order.
© 2011 PhysOrg.com