Larynx cancer treatment saves patients' voices
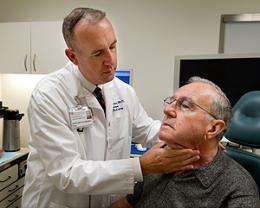
(PhysOrg.com) -- Jerry Young had had a routine endoscopy and assumed that the hoarseness that appeared in his voice was an after-effect of that exam. “If it doesn’t go away in a couple of weeks, make an appointment with an ENT,” his doctor told him. It didn’t and Young went to see an ear, nose and throat physician, who thought the redness on Young’s left vocal cord was caused by a virus.
Young was not convinced. His research made him suspect that cancer was the cause. A friend of his wife, under treatment for cancer at Stanford Hospital & Clinics, recommended he see a physician there.
His redness was cancer, a squamous cell carcinoma. It was small, at an early stage. Radiation offered as much as a 90 percent chance of removing the cancer, so Young went through that treatment. But the cancer remained and Edward Damrose, MD, director of the Stanford Voice and Swallowing Center, became Young’s doctor.
In the midst of his fear about the cancer, Young prepared himself for the worst. He didn’t think about what surgery might bring; he just wanted the cancer out. “Both my mother and brother died young, of pancreatic cancer. I knew mine was neither as aggressive or lethal as theirs, but having any kind of cancer was not something I wanted,” he said.
Young was focused more on survival than on a side effect of treatment, which leaves many such patients unable to speak without the aid of a device. But Damrose, who is also an assistant professor of otolaryngology, was concerned with both: He removed the cancer with a surgery that saved Young’s ability to speak without any kind of mechanical equipment inserted in his neck.
In a surgery done only at a few medical centers in the United States, Damrose excised the part of Young’s larynx where the cancer lay. Then he closed the gap by connecting the two main supports of the larynx, the cricoid cartilage and the hyoid bone. Instead of air vibrating through the muscular vocal cords, it vibrates with the help of cartilage, allowing for a human voice instead of a robotic one.
The procedure is called a supracricoid laryngectomy with cricohyoidoepiglottopexy. Young’s surgery was one of just a dozen times in the last year that Damrose, one of the nation’s few experts in the procedure, performed it at Stanford Hospital & Clinics.
The voice is, of course, as distinctly identifying as a person’s face. Perhaps even more than the face, the voice conveys the nuances of emotions, but, of course, it’s as an audio track, rather than a visual display.
The voice emerges from the interplay of the vocal folds, muscles, cartilages, nerves, tongue, mouth, palate and lungs. The ability to speak can be altered by a number of changes in that set of voice-enabling components, including loss of muscle mass, vocal cord atrophy or paralysis — and surgery for cancer.
Cancer of the larynx is the most commonly diagnosed head and neck cancer. Between 10,000 and 12,000 new cases arise each year in the United States. But it is the least common cause of hoarseness. Its symptoms also include difficulty swallowing, coughing up blood, sore throat and trouble breathing.
Any surgery in these tight quarters must be done precisely. “One millimeter too far one way,” Damrose said, “and you’ve cut out an important nerve needed to speak. Too far the other way and you’ve left cancer behind, or your patient will never swallow again.”
That precision, he said, is even more of a challenge because “you are cutting through thick and muscular tissue,” he said. If a patient has had radiation, that treatment can distort and swell the structures’ appearance, adding another level of difficulty.
“I had no idea that voice sparing was an option,” Young said. “Dr. Damrose just said, ‘We’ll go in and take this thing out.’ He didn’t want to get my hopes up, I think, so he didn’t get into specifics. It was months later that he asked if I wanted to know the specifics. I had no idea that he was one of the few in the U.S. with the ability and skill to do this surgery.”
The traditional approach has been to remove the entire larynx, following failed chemotherapy or radiation. It’s a relatively quick surgery — about four hours, compared with the seven hours Damrose needed for Young’s partial laryngectomy.
The impact is hugely different. With a total removal of the larynx, speaking is possible only with external help. The most common involves a prosthesis that fits into a hole in the throat; some work when pressure is applied, others can function hands-free. For others, speaking requires an electronic device pressed against the throat to amplify vocal sounds. Sometimes, some of the nerves to the tongue can be affected, damaging the ability to swallow and taste.
The psychological trauma, Young said, is immense. He saw it first when he went to a meeting of a laryngectomy support group and found himself the only person without a prosthesis. “None of the people there had ever even heard about the surgery I’d had.”
Developed in the 1950s and popularized by French surgeons, the surgery Damrose performed on Young was not done in the United States until the 1990s. And its frequency remains low. “I’d like to see this more routinely offered, to preserve more larynxes,” said Damrose. “It’s an operation that has a high degree of success and predictable results. It’s worthwhile trying.”
While a voice can undergo changes from the surgery, Young said that he is happy with the result.
It took several months for Young to discover what his new voice would sound like and to be able to make himself understood. He has a new vocal reality, a new normalcy, he calls it, with delightful wit. “My wife loves that I can’t yell at her anymore,” he said. And its deep tone, with a roughed edge, has won some admirers. “Lots of women say it’s very sexy,” Young said, with a bit of a blush.