Lactate shuttle may fuel the injured brain
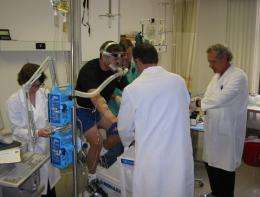
The same fundamental biological mechanism that helps athletes develop endurance on a treadmill may someday be tapped into by doctors in intensive care units to save and improve the lives of patients with traumatic brain injuries, according to research being conducted by George Brooks, a professor in UC Berkeley’s Department of Integrative Biology, in collaboration with colleagues in the Department of Neurosurgery at the University of California, Los Angeles.
An authority in the area of metabolic adjustment to exercise, Brooks developed the lactate shuttle theory, a fundamental biological mechanism that allows muscles to take up lactate via transporter proteins that “shuttle” lactate within and between cells. Inside muscle and other cells is the mitochondrial reticulum, the intracellular energy factory that uses the lactate as fuel. With sustained training, mitochondrial mass increases, burning lactate more efficiently for energy.
As it turns out, Brooks says, more recent research demonstrated that the process is not restricted to muscle tissue only.
“The same lactate transporters that we see in muscle, that change their expression with exercise training, also appear in the brain in the same kind of metabolic pathway,” he says. “The lactate shuttle occurs in the brain.”
When Brooks embarked on his pioneering research in the area of lactate metabolism nearly 40 years ago, he could not have foreseen the far-reaching applications of his work. A track runner at Queens College in the 1960s, he challenged the conventional wisdom about lactate in his controversial Ph.D. dissertation. Far from being a bane for athletes, poisoning their muscles with waste product, lactate is devoured by muscle as an efficient energy source, Brooks demonstrated.
In the decades that followed, Brooks has continued his research in his Exercise Physiology Laboratory at UC Berkeley. Here he looked at pathways for lactate formation and removal before, during and after exercise and came up with the lactate shuttle theory in 2006.
In his three-year-old collaboration with UCLA, Brooks is considering using lactate as an efficient replacement fuel for the brain in the crucial hours following a traumatic brain injury, when the brain’s ability to use glucose — considered the primary source of energy for the brain – is suppressed.
Brooks and his colleagues conducted tracer-based studies on 38 patients with traumatic brain injuries at UCLA in order to measure the amount of lactate entering and leaving their brains. The scientists labeled the lactate with C13, a non-radioactive isotope and added it to the IV solution containing isoproterenol, a synthetic epinephrine supplied to support patients’ weakened cardiovascular systems.
What they found is that during the first to 12 to 14 hours after the injury, the brain, starved for glucose, takes up lactate. “In fact, it prefers it,” Brooks says. “When blood lactate rises, the brain stops using glucose and switches to lactate. And when that happens, the patients do better.”
The question is, why? Brooks hypothesizes that the brain uses lactate more efficiently to generate energy for recovery. He points to astrocytes, star-shaped cells in the brain. “Their job is to take up glucose and bathe the neurons in lactate. And the neurons run on lactate. That’s the lactate shuttle again — the same term.”
Once Brooks can demonstrate that this lactate shuttle can be used to bypass the blockage of glucose metabolism in the brain, he will seek to support the brains of injured people with various lactate compounds, such as lactate salts and esters.
“In traumatic injuries, there is this metabolic deficit,” he says. “If we can help support the brain metabolically, maybe these people can get through.”
Conducting such research, however, is extremely difficult because of the inherent limited access to patients right now. Since the potential research subjects are unconscious, having just suffered potentially life-threatening brain injuries, their families need to be approached for permission to use the lactate markers at the worst possible time. As a result, Brooks says, their ability to conduct the studies is “episodic,” especially considering that at the moment there is no direct benefit to the patient.
“Medical boards at UC Berkeley and UCLA will have to allow us to supplement these people with lactate salts. Only then the widespread applications will be forthcoming,” Brooks says. For that to happen, he adds, “we need to show active but suppressed metabolism in the injured brain and that we can manipulate the lactate delivery to facilitate the recovery process.”
Should they be successful, this research could have far-reaching implications on how patients are treated in emergency rooms in the crucial hours after sustaining a devastating brain injury, and hopefully on their survival rates and recovery beyond.
The UCLA-UC Berkeley collaboration is only one of a number of studies being conducted at Berkeley and elsewhere that rely on the lactate shuttle mechanism. For instance, Rajaa Hussien, a graduate student in Brooks’ group, is studying lactate shuttles within cancer tumors in the hope of selectively killing the cancer cells while leaving healthy tissue intact. And Professor Song Lee in chemical engineering at Berkeley is using lactate scaffolding as a base to grow stem cells. So, rather than the 1920’s view that working muscles make and release a metabolic poison, those working muscles make a substance, lactate, that has several beneficial functions, one of which is to serve as an important energy source.
Although Brooks admits he never considered these broad applications when he started his lactate research, he is not surprised by the breadth of work that came out of research in exercise physiology.
“Lactate shuttles,” he says, “are the way nature does things.”
ScienceMatters@Berkeley is published online by the College of Letters and Science at the University of California, Berkeley. The mission of ScienceMatters@Berkeley is to showcase the exciting scientific research underway in the College of Letters and Science and the College of Chemistry.