To starve a tumor
(PhysOrg.com) -- Since the 1920s, scientists have known that cancer cells generate energy differently than normal cells, a phenomenon dubbed the 'Warburg effect' after its discoverer, German biochemist Otto Warburg. However, the field of cancer-cell metabolism has been largely ignored since the 1970s, when researchers flocked to study newly discovered cancer-causing genes.
Now a new generation of researchers is setting its sights on cancer cells’ bizarre and seemingly inefficient metabolism, which appears to be tightly linked to many of the genes already implicated in cancer.
Recent discoveries suggest that cancer cells genetically reprogram their energy-generating pathways to create the building blocks they need to grow and divide out of control, wasting a great deal of energy in the process. Potential drugs that block this pathway could offer a new way to treat a range of cancers, says Matthew Vander Heiden, assistant professor of biology and member of the David H. Koch Institute for Integrative Cancer Research at MIT.
“All tumors have to deal with shifting metabolism as they proliferate,” says Vander Heiden, who joined the Koch Institute last fall. “If you can interfere with that, you have a chance to make a difference across many tumor types.”
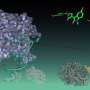
Vander Heiden is now studying one of the key enzymes involved in cancer cells’ metabolic pathways, known as pyruvate kinase M2, with an eye toward developing drugs that could alter its activity and effectively starve cancer cells of the materials they need to grow and reproduce.
Wasting energy
Human cells use sugar as an energy source, breaking it down through a series of complex chemical reactions that requires oxygen. Warburg discovered that tumor cells switch to a less efficient metabolic strategy known as fermentation, which does not require oxygen and produces much less energy.
Because they burn fuel so inefficiently, cancer cells take up more glucose than regular cells. Scientists have exploited this by using PET scans that track glucose metabolism as a diagnostic tool to reveal whether tumors have spread from their original location.
After Warburg’s initial discovery, cancer researchers spent several decades, from the 1930s to the 1960s, trying to figure out the biochemistry of cancer metabolism. But in the 1970s, the discovery of cancer-causing genes (oncogenes) and tumor suppressor genes led to the “realization that cancer is a genetic disease, not a metabolic disease like diabetes or obesity,” says Lewis Cantley, professor of systems biology at Harvard Medical School.
However, interest in cancer metabolism has surged, especially in the last few years, as evidence mounts that many of those oncogenes play a role in cancer cells’ metabolic switch. “The cancer world is full of people studying Ras [a gene that can cause cancer when mutated], p53 [a tumor-suppressor gene] and all of these different signaling and genetic things,” says Vander Heiden. “They’re all tied to metabolism in different ways.”
The cancer metabolism resurgence started gradually in the early 1990s, when Vander Heiden was a graduate student at the University of Chicago. There, he worked with Craig Thompson, one of the pioneers of the rejuvenated field. Vander Heiden soon realized that “there are still a lot of things we didn’t understand about metabolism that seemed to have been forgotten about.”
After earning his MD/PhD, Vander Heiden went to Cantley’s lab at Harvard, where he studied pyruvate kinase M2 (PKM2), which controls a key step in fermentation. In 2008, Vander Heiden, Cantley and others at Harvard Medical School reported in the journal Nature that when cells shift between normal and Warburg metabolism, they start using PKM2 instead of pyruvate kinase M1, the enzyme that most adult cells use for glycolysis (the first set of chemical reactions required to break down glucose for energy).
One major benefit of potential drugs that interfere with PKM2 is that the enzyme is not found in most normal adult cells, which could eliminate the side effects commonly seen in existing cancer drugs, says Celeste Simon, professor of cell and developmental biology at the University of Pennsylvania.
“A big problem in oncology over the past few decades is that so many of the drugs have unfortunate side effects, which limits the dosage you can administer to patients and has a major impact on quality of life,” says Simon, one of the organizers of an American Association for Cancer Research conference on cancer metabolism last fall.
A company cofounded by Cantley is now developing potential drugs that target PKM2. (Vander Heiden is a scientific advisor for the company, Agios Pharmaceuticals.)
However, PKM2 is not the only possible drug target, says Cantley. “One thing that a lot of people find attractive about targeting metabolic enzymes for drug therapy is that there are a lot of enzymes involved,” he says.
Provided by Massachusetts Institute of Technology