Virus-free technique enables scientists to easily make stem cells pluripotent
Tiny circles of DNA are the key to a new and easier way to transform stem cells from human fat into induced pluripotent stem cells for use in regenerative medicine, say scientists at the Stanford University School of Medicine. Unlike other commonly used techniques, the method, which is based on standard molecular biology practices, does not use viruses to introduce genes into the cells or permanently alter a cell's genome.
It is the first example of reprogramming adult cells to pluripotency in this manner, and is hailed by the researchers as a major step toward the use of such cells in humans. They hope that the ease of the technique and its relative safety will smooth its way through the necessary FDA approval process.
"This technique is not only safer, it's relatively simple," said Stanford surgery professor Michael Longaker, MD, and co-author of the paper. "It will be a relatively straightforward process for labs around the world to begin using this technique. We are moving toward clinically applicable regenerative medicine."
The Stanford researchers used the so-called minicircles - rings of DNA about one-half the size of those usually used to reprogram cell - to induce pluripotency in stem cells from human fat. Pluripotent cells can then be induced to become many different specialized cell types. Although the researchers plan to first use these cells to better understand - and perhaps one day treat-human heart disease, induced pluripotent stem cells, or iPS cells, are a starting point for research on many human diseases.
"Imagine doing a fat or skin biopsy from a member of a family with heart problems, reprogramming the cells to pluripotency and then making cardiac cells to study in a laboratory dish," said cardiologist Joseph Wu, MD, PhD. "This would be much easier and less invasive than taking cell samples from a patient's heart." Wu is the senior author of the research, which will be published online Feb. 7 in Nature Methods. Research assistant Fangjun Jia, PhD is the lead author of the work.
Longaker is the deputy director of Stanford's Institute for Stem Cell Biology and Regenerative Medicine and director of children's surgical research at Lucile Packard Children's Hospital. Wu is an assistant professor of cardiology and of radiology, and a member of Stanford's Cardiovascular Institute. A third author, Mark Kay, MD, PhD, is the Dennis Farrey Family Professor in Pediatrics and professor of genetics.
The finding brings together disparate areas of Stanford research. Kay's laboratory invented the minicircles several years ago in a quest to develop suitable gene therapy techniques. At the same time, Longaker was discovering the unusual prevalence and developmental flexibility of stem cells from human fat. Meanwhile, Wu was searching for ways to create patient-specific cell lines to study some of the common, yet devastating, heart problems he was seeing in the clinic.
"About three years ago Mark gave a talk and I asked him if we could use minicircles for cardiac gene therapy," said Wu. "And then it clicked for me, that we should also be able to use them for non-viral reprogramming of adult cells."
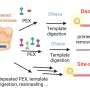
The minicircle reprogramming vector works so well because it is made of only the four genes needed to reprogram the cells (plus a gene for a green fluorescent protein to track minicircle-containing cells). Unlike the larger, more commonly used DNA circles called plasmids, the minicircles contain no bacterial DNA, meaning that the cells containing the minicircles are less likely than plasmids to be perceived as foreign by the body. The expression of minicircle genes is also more robust, and the smaller size of the minicircles allows them to enter the cells more easily than the larger plasmids. Finally, because they don't replicate they are naturally lost as the cells divide, rather than hanging around to potentially muck up any subsequent therapeutic applications.
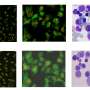
The researchers chose to test the reprogramming efficiency of the minicircles in stem cells from human fat because previous work in Wu and Longaker's lab has shown that the cells are numerous, easy to isolate and amenable to the iPS transformation, probably because of the naturally higher levels of expression of some reprogramming genes. They found that about 10.8 percent of the stem cells took up the minicircles and expressed the green fluorescent protein, or GFP, versus about 2.7 percent of cells treated with a more traditional DNA plasmid.
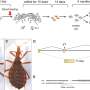
When the researchers isolated the GFP-expressing cells and grew them in a laboratory dish, they found that the minicircles were gradually lost over a period of four weeks. To be sure the cells got a good dose of the genes, they reapplied the minicircles at days four and six. After 14 to 16 days, they began to observe clusters of cells resembling embryonic stem cell colonies - some of which no longer expressed GFP.
They isolated these GFP-free clusters and found that they exhibited all of the hallmarks of induced pluripotent cells: they expressed embryonic stem cell genes, they had similar patterns of DNA methylation, they could become multiple types of cells and they could form tumors called teratomas when injected under the skin of laboratory mice. They also confirmed that the minicircles had truly been lost and had not integrated into the stem cells' DNA.
Altogether, the researchers were able to make 22 new iPS cell lines from adult human adipose stem cells and adult human fibroblasts. Although the overall reprogramming efficiency of the minicircle method is lower than that of methods using viral vectors to introduce the genes (about 0.005 percent vs. about 0.01-0.05 percent, respectively), it still surpasses that of using conventional bacterial-based plasmids. Furthermore, stem cells from fat, and, for that matter, fat itself, are so prevalent that a slight reduction in efficiency should be easily overcome.
"This is a great example of collaboration," said Longaker. "This discovery represents research from four different departments: pediatrics, surgery, cardiology and radiology. We were all doing our own things, and it wasn't until we focused on cross-applications of our research that we realized the potential."
"We knew minicircles worked better than plasmids for gene therapy," agreed Kay, "but it wasn't until I started talking to stem cell people like Joe and Mike that we started thinking of using minicircles for this purpose. Now it's kind of like 'why didn't we think of this sooner?'"
Provided by Stanford University Medical Center