Dead neuron clean-up crew in peripheral nervous system found
(PhysOrg.com) -- Death is messy, especially in the developing nervous system. During embryonic development, more nerve cells (neurons) are produced than we will ever need or use. About half of those unnecessary neurons die through a pre-programmed "suicide” mechanism called apoptosis.
That leaves a lot of dead neurons lying around. And the decaying "corpses” of these neurons, if not cleared, could cause the body's immune system to go into overdrive, instigating autoimmune conditions.
So disposing of these neuronal corpses is essential for a healthy nervous system. But surprisingly little is known about the disposal processes.
Bruce Carter and colleagues have now identified members of the "clean-up crew” — including a protein named Jedi-1 — responsible for getting rid of the corpses of dead sensory neurons in the peripheral nervous system of mouse embryos. Their findings, in the December issue of Nature Neuroscience, could hold important implications for autoimmune disease.
"There is a lot of data about how neurons die during development,” says Carter, a professor of biochemistry who has been studying apoptosis since the early 1990's. "But the idea that something has to be done to get rid of the dead neurons wasn't something we had thought about.”
In the brain and spinal cord (the central nervous system, or CNS), the debris of dead neurons is primarily cleared by microglia — specialized immune cells that reside only in the CNS. Some studies suggested that glia, another type of non-neuronal cell that support and protect neurons, might be also important.
But less is known about the process in the peripheral nervous system (PNS) — the nerves outside the brain and spinal cord. "Which is really surprising because we've known about programmed cell death in the peripheral nervous system for 70 years,” says Carter.
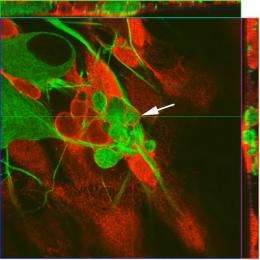
Carter's lab began looking for the cells responsible for this clean up in the PNS of the mouse embryo. They found that, in the mouse dorsal root ganglia — clusters of neurons near the spinal cord — the dead neurons were engulfed almost exclusively by "satellite glial cell precursors.”
Satellite glial precursors surround nerve cells in the developing PNS and, at later stages of development, can become either mature satellite glia or Schwann cells, which create the insulating myelin sheath that surrounds peripheral nerves.
Scavenging for and disposing of dead cells is not the primary role of these cells, explained Jami Scheib, a graduate student in the Carter lab and co-author on the paper. Other cell types, like macrophages and microglia, are the body's "professional” phagocytes — cells that eat foreign particles and cellular debris.
Unlike macrophages and microglia, "satellite glial cell precursors are 'amateur' phagocytes because they have other jobs (in the nervous system), like keeping the environment around neurons healthy,” Scheib says.
Having identified the cells responsible for clearing dead neurons, Carter's group began looking for the molecular mediators of the clearance process.
Hsiao-Huei Wu, a postdoctoral fellow in Carter's lab at the time, searched gene databases for mammalian genes that might encode "engulfment receptors” — proteins that recognize the "eat me” signals on dying cells. She found three mammalian genes that were similar to known engulfment receptors in other species: MEGF10, MEGF11 and MEGF12, also known as Jedi-1.
Wu and Scheib then demonstrated that two of them — MEGF10 and Jedi-1 — were expressed in the satellite glial cell precursors and that both could bind to the mouse neuronal corpses, suggesting that MEGF10 and Jedi-1 could be acting as engulfment receptors.
Additionally, expressing Jedi-1 or MEGF10 in fibroblasts — cells that don't normally function as phagocytes — facilitated binding to dead neurons. Conversely, blocking expression of these proteins in glial cells inhibited their ability to engulf dying neurons, providing further support that Jedi-1 and MEGF10 function as engulfment receptors.
The findings suggest a cellular and molecular mechanism for how the mammalian body disposes of neuronal corpses during development, which might have implications for understanding the development of autoimmune diseases.
"The prediction is that you could develop an inflammatory response over time if these dead cells are sitting around, which would increase the risk of autoimmune disease,” Carter says.
Scheib is continuing to pursue the molecular mechanisms to answer questions like: if Jedi-1 is a receptor, what does it do? And why are there two receptors? Do they work together?
Carter's group is also knocking out Jedi-1 in the glial precursor cells of mice to see if the mice develop autoimmune conditions and investigating whether the same processes are involved in clearing the cellular "waste” after nerve injury.
More information: www.nature.com/neuro/index.html