HIV-1 damages gut antibody producing immune cells within days of infection
The virus that causes AIDS is classified as a lentivirus, a word derived from the Latin prefix, "lenti-," meaning "slow." But new research from the NIAID-funded Center for HIV/AIDS Vaccine Immunology suggests that HIV-1 is anything but - moving at breathtaking speed in destroying and dysregulating the body's gut-based B-cell antibody-producing system.
"These new data show that damage to the antibody arm of the immune system begins quickly, within days. We know that by 80 days, half of the generative microenvironments for antibodies within the immune system in the gut are destroyed," said Barton Haynes, M.D., director of the Center for HIV/AIDS Vaccine Immunology and the senior author of the study.
The study, published in the open access journal PLoS Medicine at
http://medicine.plosjournals.org/perlserv/?request=get-document&doi=10.1371/journal.pmed.1000107, is the first to examine what happens to B cells in the gut in the earliest stage of HIV-1 infection. Researchers say the findings may shed light on one of the big mysteries in HIV: why the B cell, or antibody response, is so slow to arise - and so weak when it finally does, that it is unable to offer any kind of meaningful defense.
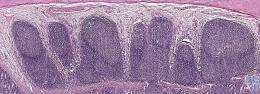
B cells that make antibodies against invading microbes are born in the bone marrow but migrate out and mature in different locations throughout the body. Some wind up in the intestine and settle in stretches of lymph node-like follicles called Payer's patches that are found at the bottom of the small intestine.
There, tucked inside the follicles' nurturing germinal centers, the B cells set up surveillance, waiting to rise up against incoming bacteria, viruses, or other pathogens. "Unfortunately, we found they are no match for HIV-1," said Anthony Moody, M.D. a member of the Duke Human Vaccine Institute (DHVI) and a lead author of the study.
Moody and co-lead author Marc Levesque, M.D., a former member of DHVI but now at the University of Pittsburgh, led a team of researchers in examining B cells in blood as early as 17 days after viral transmission, and in lymph tissue in the gut beginning at 47 days after transmission in 40 people infected with HIV-1. They compared their findings with similar tissue from healthy controls.
They discovered that even at this early stage, HIV-1 had already ravaged the gut's B cell arm of the immune system. The vast majority of the follicles in the Payer's patches had been damaged. "HIV-1 turns on the immune system, but turns it on in the wrong way," Moody said. "We found that it was churning out all sorts of B cells. Some appeared to be reactive against HIV-1, but others appeared reactive to things like influenza as well as self molecules."
In addition, the researchers found that by as early as 17 days after transmission, HIV-1 decreased the numbers of naďve B cells - cells that may have had the potential to mature into potent infection-fighters.
Such deregulation had been described in chronic HIV-1-infection, but never before in such an early phase of the disease, said Moody. "It is no wonder the B cell response is so weak in response to HIV-1 infection. The virus causes such early disruption that it is simply not able to work as it is supposed to. "It is really quite sobering."
The findings may be sobering, but they also reinforce the research team's vision of what a successful AIDS vaccine might look like.
"First, an effective vaccine will have to produce potent antibodies that would already be in circulation before infection occurs," said Haynes, who is also a professor of medicine and director of the Human Vaccine Institute at Duke. "Then, if the virus manages to escape that first line of defense, the vaccine would need to be able to educate the immune system to rapidly respond to eliminate transmitted virus strains. It is this continually emerging picture of what happens at the very earliest period after infection that is helping us to understand the job we have to do," Haynes said.
Source: Duke University Medical Center (news : web)















