Engineered bacterium churns out two new key antibiotics
(PhysOrg.com) -- In recent years, scientists have isolated two potent natural antibiotics — platensimycin and platencin — that are highly effective against bacterial infection, including those caused by the most dreaded drug-resistant microbes.
Now, those two promising agents are a key step closer to augmenting a depleted antibiotic pipeline with the discovery of a genetic pressure point that can send a bacterium that makes both antibiotics into overdrive.
In a report in the online editions of the journal Antimicrobial Agents and Chemotherapy, a team led by University of Wisconsin-Madison professor of pharmaceutical sciences and chemistry Ben Shen shows that a South African soil microbe can be engineered by manipulating a single gene to make large amounts of both antibiotics.
"There is no doubt about the importance of these compounds," says Shen, who conducted the work with colleagues Michael J. Smanski, Ryan M. Peterson and Scott R. Rajski. "They are active on all the drug-resistant bacterial pathogens."
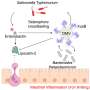
The compounds are among the first discovered in the past 40 years that represent a new class of antibiotics and that exhibit a new mode of action. They work by targeting an enzyme used to make the fatty acids critical for building the cell membranes on the surface of pathogenic bacteria. The need for new antibiotics is significant and growing as pathogenic bacteria are evolving resistance to currently available antibiotics, with some infections becoming almost impossible to treat.
The new Wisconsin discovery is notable because it provides a blueprint for the manufacture of large amounts of antibiotic, a key step in the commercial development of any drug. The team showed that a liter of the engineered bacterium Streptomyces platensis can churn out as much as 300 milligrams of antibiotic, more than 100 times the amount produced by wild strains of the bacterium.
"That's a lot of material," says Shen. "We didn't even optimize production."
The ability to produce large amounts of the new antibiotics, which to date have only been tested in animals, should help speed the development of the new antibiotics, as they are difficult to produce by conventional means.
The compounds, Shen explains, work well in animals when administered by continuous infusion, but their efficacy is diminished when administered by more conventional means. That phenomenon, Shen notes, is attributed to properties associated with how the agents are processed by an animal. It may be possible, however, to improve those properties by chemical modification of the natural antibiotics, a process that can now be accelerated in the lab as researchers will have greater access to the new agents through the engineered bacterium developed by the Wisconsin team.
The new work by Shen and his colleagues also lays a foundation to develop analogs, compounds that have improved properties as a result of tinkering with the biosynthesis pathways used by the engineered bacterium to make the antibiotics.
The conversion of ordinary Streptomyces platensis into a lean, mean antibiotic-producing machine required the manipulation of only a single regulatory gene, according to the new study. By deleting the gene from the bacterium that produces the compounds, the Wisconsin team was able to find strains of the bacterium that overproduced the antibiotics.
The new study was funded by UW-Madison and the National Institutes of Health.
Provided by University of Wisconsin-Madison