New approach to genetic testing could halve deaths from inherited bowel cancer
Changing the approach to genetic screening for cancers in Australia could effectively halve deaths caused by an inherited form of bowel cancer, says a University of Melbourne expert.
Professor John Hopper – an Australia Fellow of the National Health and Medical Research Council in the Melbourne School of Population Health –says current cancer genetic screening programs are highly focused on breast cancer and typically based on family history alone.
But studies in the UK and Australia have now shown that most of the women who have been tested had a low chance of carrying a faulty gene which causes cancer.
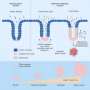
Instead, he says, genetic screening should focus more on testing the tumors of young people who develop cancers to determine if they are caused by an inherited genetic fault which might be shared by other family members.
"If we redirect the emphasis of our genetic screening programs to focus more on people who already have cancer we can make a really big difference,'' he says.
"We can work with patients to help prevent them developing new cancers, or at least detect them at an early stage, and we can arm their families with the knowledge to help save lives."
Professor Hopper says that in the case of bowel cancer, deaths caused by an inherited form of the disease could effectively be halved if the tumors of early-onset cancer sufferers were routinely tested for signs of an inherited genetic cause.
"We now have evidence from studies carried out in Australia and elsewhere that show how to do this in the most cost-effective manner,'' he says.
"Relatives of the patient could, if they wished, then also be tested for the same genetic fault.
"Those who were found to be carriers could then receive regular bowel screenings to detect early signs of any cancers and greatly reduce their chance of dying from the disease."
Bowel cancer is one of the most common forms of cancer in Australia. There are about 1000 cases each year diagnosed in people under the age of 50, and about 10 per cent of these (100 per year) are the result of genetic fault that can now be detected.
Professor Hopper says a similar approach could also be taken to improve genetic testing for breast cancer by studying the tumors of young women who developed the disease.
"Breast cancers arising in young women with an inherited fault in BRCA1 have particular features that pathologists can easily identify,'' he says.
"Women with an inherited fault in BRCA1 have about a 60 per cent lifetime risk of developing breast cancer, and a 40 per cent lifetime risk of developing ovarian cancer."
Professor Hopper says it would still be appropriate to offer genetic testing to people with a very strong family history of breast or bowel cancers, especially if it involved diagnoses before the age of 50.
"However, those who have a low chance of carrying a genetic risk can now be easily identified by genetic counsellors and reassured."
Source: University of Melbourne