Prostate cancer genes behave like those in embryo
Gene activity in prostate cancer is reminiscent of that in the developing fetal prostate, providing further evidence that all cancers are not equal, Johns Hopkins researchers report. The finding could help scientists investigate how to manipulate the genetic program to fight a disease whose biology remains poorly understood despite more than half a century of investigation.
Decades ago, researchers noticed that cancers often display many of the same "forever young" features seen in healthy embryonic organs during their early development: fast growth, evasion of aging and death, recruitment of blood vessels to grow more tissue, lots of movement and invasion of nearby tissue.
Though researchers noticed these similarities as far back as the 1920s, the sophisticated technology necessary to test the relationships between development and cancer didn't exist until recently, says David Berman, M.D., associate professor of pathology, oncology and urology at the Johns Hopkins School of Medicine.
In a new study published online this week in Oncogene, Berman and his team used new gene-profiling technology to compare the normally developing prostate in mice to human prostate cancers. The work took advantage of extensive existing knowledge about prostate development in mouse embryos.
Male mice develop prostate glands in response to androgens - male hormones that include testosterone - during day 17 of a 21-day gestation. An absence of androgen in female mice causes the cells in the same area to develop into a vagina and urethra, but females can grow prostates if they are artificially supplied with androgen.
To kick-start prostate development on a precisely timed schedule, the researchers gave pregnant mice androgen shots on day 16 after conception, sending male hormone circulating through the mothers' bloodstreams to their developing litters. A second group of pregnant mice were injected with an inactive solution for comparison.
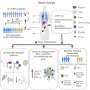
Using mouse gene chips that catalog nearly every gene in the mouse genome, the researchers probed to see which genes were turned on in the urogenital areas of developing female mice six and 12 hours after they were exposed to androgen. They also compared normally developing females (not exposed to androgen) and males (which make their own androgen).
Their gene-profiling results showed that the pattern of activity of genes presumed to be turned on and off by androgen exposure changed dynamically over time. At six hours after injection, 693 genes responded to androgen, mostly by turning off. A little later on - at 12 hours - 177 genes responded, mostly by turning on. By 48 hours, on and off responses were approximately equal, with 829 genes responding to androgen.
"Our pet theory is that these developmental genes may be first turning off normal female development in response to androgens and then turning on prostate development," says Berman. "And when we looked closer at the nature of these genes we found that many are involved in cell survival, growth and movement, which are behaviors seen in cancer cells, so we probed further to see if these genes could be directly linked to prostate cancer."
By comparing the list of mouse genes to genes whose human counterparts are known to be involved in prostate cancers, the researchers found that many of these developmental genes appear to be turned on or off in prostate cancers, especially the more aggressive types and at critical transition points during cancer progression. Moreover, says Berman, the same genes that appear to cause cells to divide, move and change shape to form the prostate in a developing fetus also seem to be reactivated in prostate cancer cells, potentially causing them to divide, move and spread.
"We've identified the programs that form the prostate in the embryo and found them to be remarkably similar to those that form tumors in prostate cancer patients," says Berman. "Since prostate development is reproducible, genetically and pharmacologically tractable, and reflects the entire spectrum of human prostate cancer progression, this gives us a new roadmap for better understanding this particular cancer and identifying new prostate cancer-specific treatments."
Source: Johns Hopkins Medical Institutions