Students invent protective pouch to enhance cell therapy

Johns Hopkins undergraduates have invented a device to improve cell therapy for diabetes patients by anchoring transplanted insulin-producing cells inside a major blood vessel.
A team of five seniors and two freshmen, working with Johns Hopkins doctors and engineers, devised a protective "pouch" that should fit inside the portal vein, which feeds into the liver. This pouch would keep microcapsules of therapeutic cells in one place, allowing them to thrive and send out needed insulin. The inventors say the same approach could be used in cell therapy for other ailments, including liver disease.
"I think it's a brilliant idea," said one of the project's sponsors, Jeff W. M. Bulte, director of the Cellular Imaging Section in the Johns Hopkins Institute for Cell Engineering.
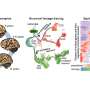
The pouch is formed by sandwiching a porous band of nylon mesh between two concentric metal stents, similar to the ones used to keep clogged blood vessels open. Once the stents are in place, microcapsules filled with helpful cells are injected into the gap between the stents, where they become trapped within the nylon mesh. Blood flowing through the vessel should nourish the encapsulated cells and circulate the proteins, such as insulin, produced by these cells.
The project is important because it could lead to better results from cellular therapy, in which live cells are injected to repair or replace damaged or depleted tissue. "It’s a device," Bulte said, "that allows the microcapsules to be removed and reinserted if additional therapy is needed – a ‘yearly refill,’ for example – and the students have provided an ideal environment in which the encapsulated cells can thrive."
Along with other undergraduate projects, this prototype was unveiled May 2 at the university’s Biomedical Engineering Design Day showcase. The Johns Hopkins Technology Transfer staff has applied for a provisional patent. Animal testing is expected to begin this summer. If it is successful, human trials would follow.
"It’s very impressive," said Aravind Arepally, an interventional radiologist who served as the project’s other sponsor. "We’re basically creating a small bio-reactor inside the vein to produce insulin and other proteins that the body needs. The students have built a housing in which the bio-reactor can operate. I’m pretty optimistic that it will work in living subjects."
The leader of the student design team, Tom Link, said he selected this project because it has the potential to benefit many people. "It could provide an important new way to treat diabetes and fulminant liver failure," said Link, 22, of Holbrook, N.Y. "I know about the health problems associated with diabetes because my grandmother has it, and she has to give herself several shots a day. If it works, this cell therapy could eliminate the need for that."
Progress in cell therapy has been slow for several reasons. First, the injected cells are often attacked by a patient’s immune system. Also, the injected cells cannot survive long without plentiful oxygen and nutrients, which are not available throughout the body. Finally, once they are inside the patient, the injected cells need to settle in a place where they can provide effective treatment without interfering with healthy body functions.
Arepally and Bulte have overcome some of these hurdles by working with semi-permeable alginate microcapsules – tiny spheres that surround the injected cells and protect them from the body’s immune system. At the same time, the spheres allow beneficial proteins to flow out and oxygen and glucose to flow freely in. Arepally and Bulte, both faculty members in the Russell H. Morgan Department of Radiology and Radiological Science of the Johns Hopkins School of Medicine, also have developed ways, covered by a pending patent, to track the microcapsules with various imaging technologies.
They and researchers elsewhere have struggled, however, to keep these encapsulated cells alive within the body, mainly because the cells often situate themselves where they do not have access to a plentiful blood supply. To address this challenge, the radiologists last year asked undergraduates in the university’s BME Design Team course to devise a way to keep the microcapsules in one place where their cells could thrive and deliver effective therapy.
During the past school year, the engineering students researched the topic, tested biomaterials and constructed the prototype, designed to fit inside the portal vein. This large blood vessel, about the diameter of an index finger, carries blood from the digestive system into the liver.
The pouch components are made to be compressed and inserted with catheters that a physician can snake into the abdomen through the femoral vein in the leg. Using real-time imaging technology, an interventional radiologist can view and guide the minimally invasive procedure as it takes place. First, the doctor would insert the stainless steel outer stent, which would push out harmlessly on the elastic interior of the vein. Next, the doctor would insert the inner stent, surrounded by the porous nylon mesh. The inner stent is made of nitinol, a metal that snaps back into its original shape after being compressed for insertion. The inner stent matches the interior diameter of the vein. When all of the pieces are inserted, the nylon mesh is held snugly against the inner stent. A gap forms between the mesh and the outer stent, allowing blood to pass through.
At this point, the physician would use another catheter to inject the encapsulated cells between the stents, where the mesh would hold them in place. The tiny openings in the mesh, each about 250 microns in diameter, would allow blood to pass through to nourish the cells and disperse helpful proteins. But the openings are too small to allow the microcapsules to escape.
In lab tests using latex tubing to represent a vein, the students used ultrasound imaging to confirm that fluid can flow smoothly through the mesh and can spread the microcapsules throughout pouch. They also demonstrated that the device causes no pressure drop in the model blood vessels and that the microcapsules can easily be injected and withdrawn.
Link said he and his team members appreciated the chance to solve a real-world engineering challenge while drawing on the expertise of prominent researchers such as Arepally and Bulte. "I don’t think I could have found an opportunity like this anywhere else," he said. "That’s one of the major strengths of Johns Hopkins." Link plans to continue working on the project in the university’s biomedical engineering master’s degree program.
Source: Johns Hopkins University