Human testis harbors HIV-1 in resident immune cells
Researchers have demonstrated HIV replication within resident immune cells of the testis, providing an explanation for the persistence of virus in semen even after effective highly active antiretroviral therapy. The related report by Roulet et al., “Susceptibility of human testis to human immunodeficiency virus-1 infection in situ and in vitro,” appears in the December issue of The American Journal of Pathology.
According to the most recent World Health Organization data, 39.5 million people are infected with HIV. Semen remains the main means of spreading the virus, even though highly active antiretroviral therapy (HAART) can successfully suppress virus in the blood. The presence of HIV in the semen despite successful HAART has intrigued scientists.
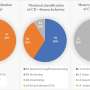
Researchers led by Dr. Nathalie Dejucq-Rainsford examined testis tissue for the presence of HIV receptors. They found that all of the necessary cellular receptors (CD4, CXCR4, CCR5, and DC-SIGN) were present on cells located within the testis, specifically testicular macrophages.
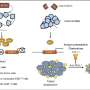
The point was demonstrated further by using explanted organ cultures in which human testis tissue was grown in culture. This testis culture, which retained the same tissue architecture as in vivo tissue and continued to secrete testosterone, was able to support infection by HIV-1. Virus produced from the testis culture was fully active as collected virus was able to infect permissive cells in culture.
The finding that HIV-1 can replicate within testicular macrophages is significant because the testis represents a pharmacological sanctuary—many anti-retroviral drugs have difficulty penetrating this organ and may be present at sub-therapeutic levels. Thus, although HAART may achieve undetectable virus levels in the blood, virus replication in the testis may permit continued spread of the virus.
Finally, with HIV infection continuing to rise, the development of anti-retroviral therapy that effectively targets all sources of HIV, including the testis, is gravely needed. The use of this testis culture system may allow assessment of new anti-retroviral drugs that target HIV in the testis.
Source: American Journal of Pathology