Heat halts pain inside the body
The old wives' tale that heat relieves abdominal pain, such as colic or menstrual pain, has been scientifically proven by a UCL (University College London) scientist, who will present the findings today at the Physiological Society's annual conference hosted by UCL.
Dr Brian King, of the UCL Department of Physiology, led the research that found the molecular basis for the long-standing theory that heat, such as that from a hot-water bottle applied to the skin, provides relief from internal pains, such as stomach aches, for up to an hour.
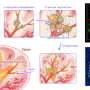
Dr King said: "The pain of colic, cystitis and period pain is caused by a temporary reduction in blood flow to or over-distension of hollow organs such as the bowel or uterus, causing local tissue damage and activating pain receptors.
"The heat doesn't just provide comfort and have a placebo effect – it actually deactivates the pain at a molecular level in much the same way as pharmaceutical painkillers work. We have discovered how this molecular process works."
If heat over 40 degrees Celsius is applied to the skin near to where internal pain is felt, it switches on heat receptors located at the site of injury. These heat receptors in turn block the effect of chemical messengers that cause pain to be detected by the body.
The team found that the heat receptor, known as TRPV1, can block P2X3 pain receptors. These pain receptors are activated by ATP, the body's source of energy, when it is released from damaged and dying cells. By blocking the pain receptors, TRPV1 is able to stop the pain being sensed by the body.
Dr King added: "The problem with heat is that it can only provide temporary relief. The focus of future research will continue to be the discovery and development of pain relief drugs that will block P2X3 pain receptors. Our research adds to a body of work showing that P2X3 receptors are key to the development of drugs that will alleviate debilitating internal pain."
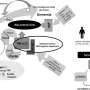
Scientists made this discovery using recombinant DNA technology to make both heat and pain receptor proteins in the same host cell and watching the molecular interactions between the TRPV1 protein and the P2X3 protein, switched on by capsaicin, the active ingredient in chilli, and ATP, respectively.
Source: University College London